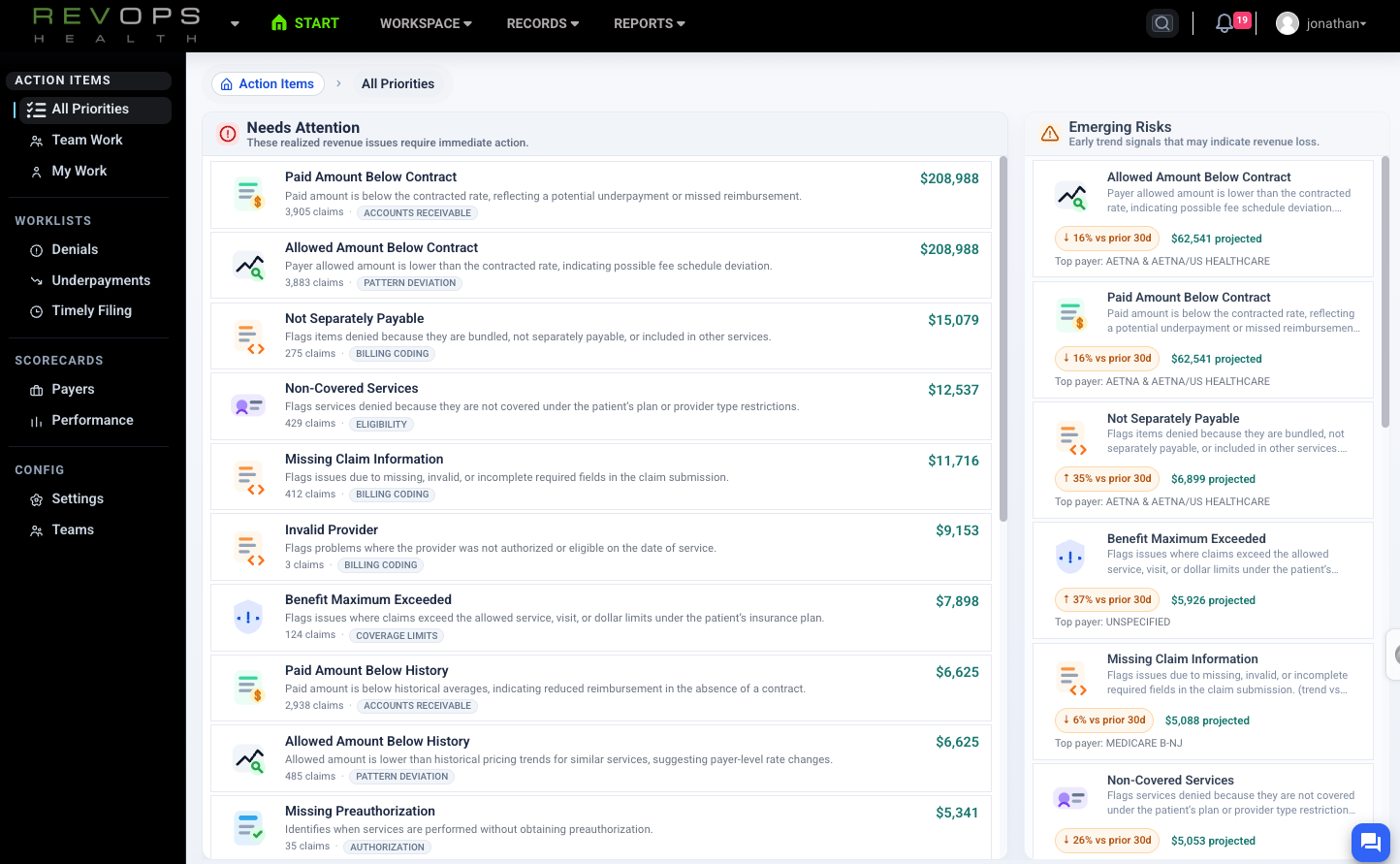
See exactly how your practice is getting paid. In real time.
Gain financial predictability without needing to be a revenue cycle expert.
RevOps Health unifies claims, remittances, and payment data into a single live view so you can understand performance, quantify risk, and make confident financial decisions.
Trusted by independent clinics, provider groups, specialty practices, and small to mid size hospitals across the United States.




Why executives choose RevOps Health




Healthcare revenue has become harder to predict.
Payer behavior changes without warning.
Reporting arrives too late to act.
And leaders are forced to rely on anecdotes instead of evidence.
RevOps Health turns opaque revenue operations into clear, quantified insight you can trust.
What RevOps Health makes possible
Know where revenue is leaking
Quantify underpayments, missed claims, and false denials so issues are prioritized by financial impact.
Understand payer behavior
Detect changes in reimbursement patterns early and hold payers accountable with evidence.
Make confident decisions
Benchmark performance, validate vendors, and allocate resources based on real data, not guesswork.

How it works

Unify your data
Claims, remittances, and payments are ingested automatically with no operational disruption.

Surface risk and impact
AI powered surveillance identifies anomalies, patterns, and financial exposure in real time.

Guide action
Issues are ranked by dollar impact so teams focus on what matters most.
Executive Buyer FAQs

-
Most reporting tools show one slice of the picture—claims, remits, or payer summaries—often limited to what the PM system exposes. RevOps blends claims, remittances, and supporting data into a single source of truth and treats claim and EOB data as the ultimate record of how you actually get paid. This allows us to identify patterns and issues that siloed reports simply cannot surface.
-
Revenue stability comes from knowing where to focus. RevOps organizes RCM activity into clear, thematic problem areas and quantifies their financial impact, allowing leaders to prioritize the highest-value opportunities. Instead of chasing issues linearly, teams can resource the biggest drivers of risk and recovery with confidence.
-
RevOps immediately surfaces common high-impact issues like underpayments, low pays, authorization failures, payer behavior shifts, and denial patterns. As the system learns each customer’s data, it quickly isolates more nuanced issues across locations, providers, specialties, service codes, and payers—often ones the organization didn’t know to look for.
-
We load historical data at go-live, so customers begin identifying and scoping problems immediately. ROI starts on day one because visibility, prioritization, and measurement begin immediately—even if cash recovery follows payer and patient payment cycles. You can’t fix what you can’t measure, and RevOps makes that measurement available from day one.
-
Yes. RevOps quantifies both volume and real-world dollars at stake by blending claims, remittances, and—when available—contractual fee schedules. This allows leaders to evaluate performance based on expected collectable revenue, not just billed amounts, and clearly understand the financial impact of execution across teams or vendors.
-
At its core, RevOps scopes problems, quantifies impact, and shows volume and trend over time. This creates guardrails around decision-making, allowing leaders to allocate resources to the highest-return initiatives instead of guessing or reacting. Every decision is grounded in measurable financial outcomes.
-
RevOps is designed for every level. Executives get top-down visibility into projects, performance, and trends. Managers see workload, throughput, and emerging issues across teams. Individual contributors can drill from high-level analytics down to specific claims and remittances. Role-based access control ensures data is shared appropriately and securely.
-
Pricing is straightforward and scales linearly based on the number of billing providers or clinics (for urgent care and ASCs). You only pay for what you use—if you grow, pricing grows with you; if you contract, pricing adjusts downward. Enterprise and hospital systems can discuss volume-based pricing.
-
RevOps enables leaders to frame decisions around clearly scoped projects with quantified financial impact. Instead of debating anecdotes or estimates, boards and ownership can evaluate initiatives based on measurable opportunity, resource requirements, and expected outcomes—making investment decisions far more defensible and data-driven.
-
RevOps replaces manual data aggregation—not expertise. It is a read-only system designed to eliminate the grind of assembling reports while enabling deeper analysis through search, pattern detection, and evidence-backed outputs. Internal teams and consultants can focus on solutions and execution, while RevOps provides the data, monitoring, and feedback loop to track progress over time.

Get clarity into your revenue cycle
Understand how you are getting paid, what is at risk, and where to focus next.








