REAL TIME CLARITY FOR YOUR ENTIRE REVENUE CYCLE
The RevOps Health platform gives clinics and provider groups a single platform that blends claims, remittances, and payer behavior into one real time view. Teams uncover lost revenue, detect payer anomalies early, and make confident decisions backed by data.
REVENUE CYCLE TEAMS ARE EXPECTED TO SOLVE PROBLEMS THEY CANNOT SEE
LIMITED VISIBILITY
Leadership relies on delayed or incomplete reporting, which makes it difficult to see what is happening in real time or make confident decisions.
REACTIVE WORKFLOWS
Managers spend hours gathering data and chasing issues, often discovering problems only after they affect cash flow and disrupt daily operations.
FRAGMENTED SYSTEMS
Claims, remittances, and practice data sit in separate systems, hiding payer behavior patterns and slowing the analysis teams need to stay ahead.
MANUAL INVESTIGATIONS
Analysts struggle with rigid tools and manual exports that make tracing anomalies slow, difficult, and dependent on time consuming spreadsheets.
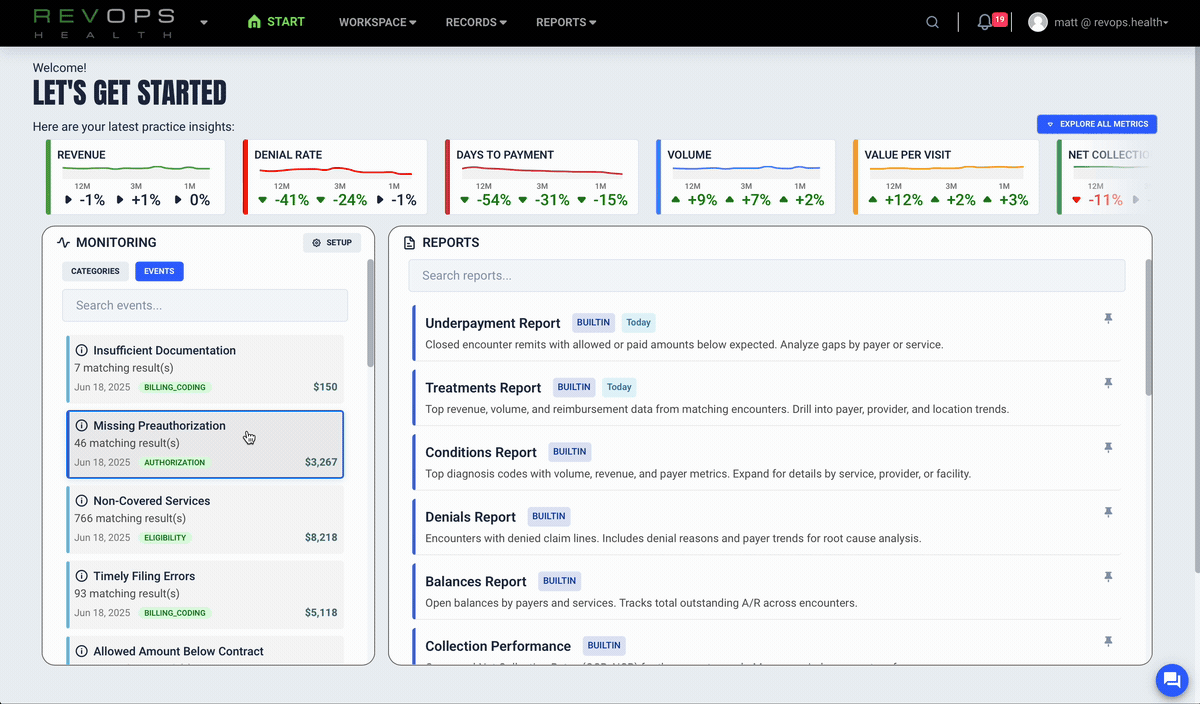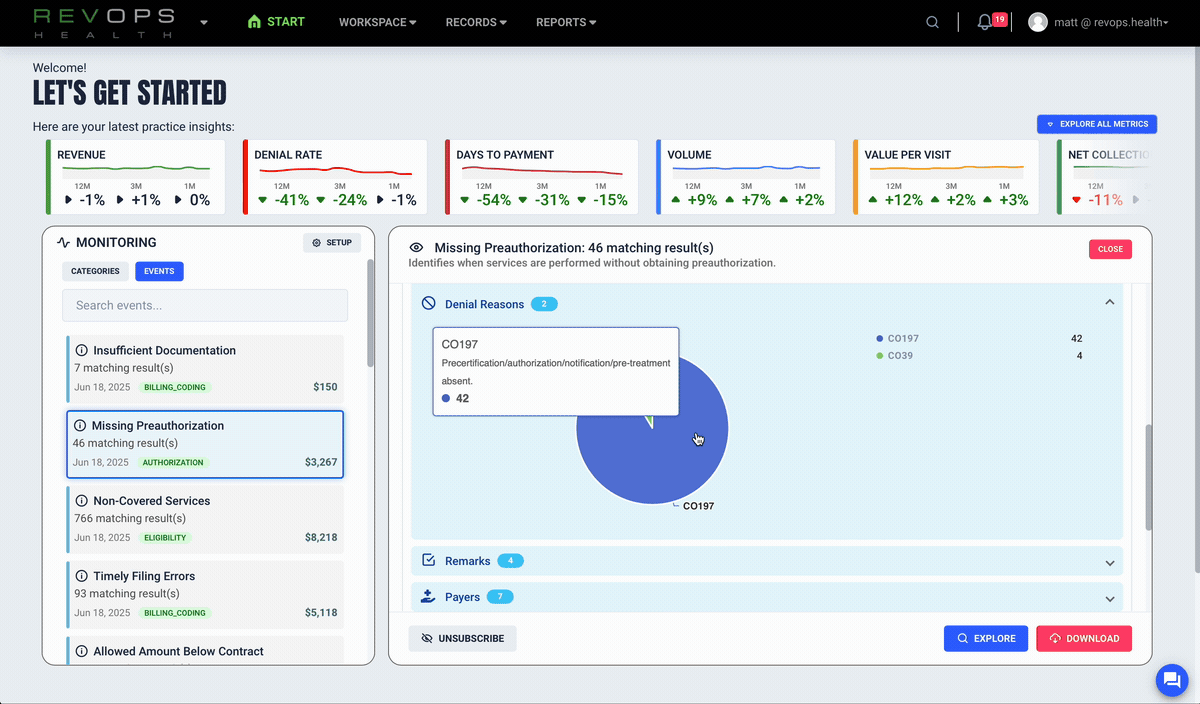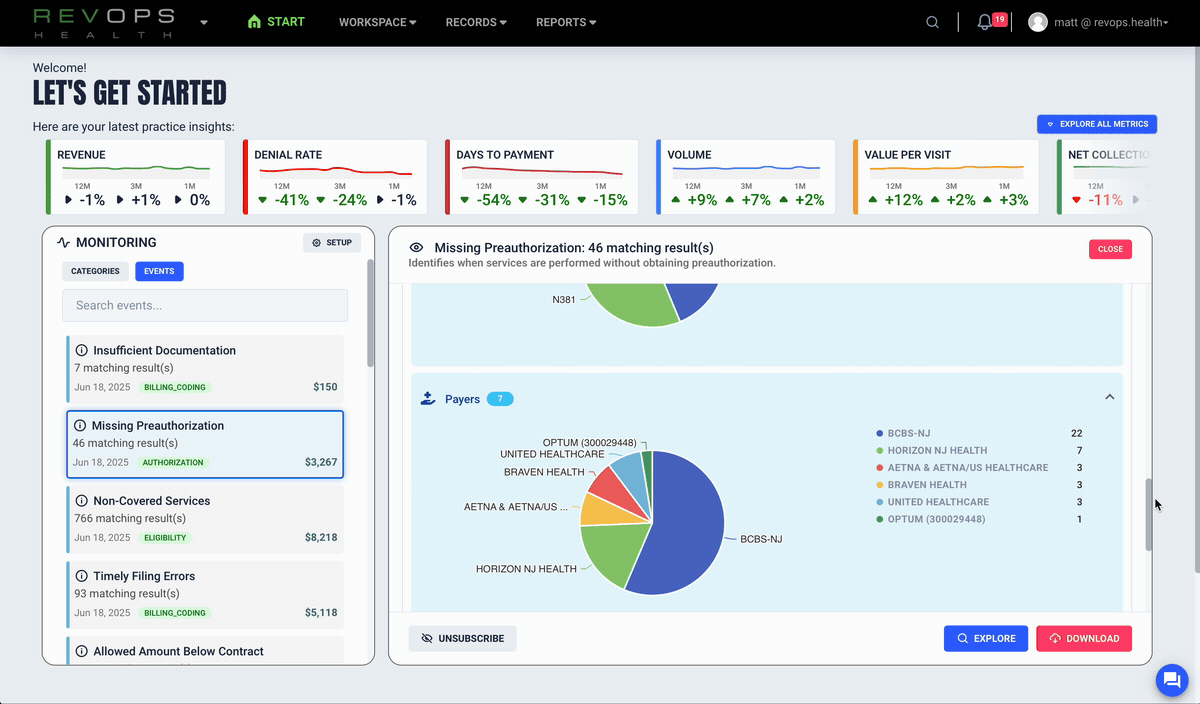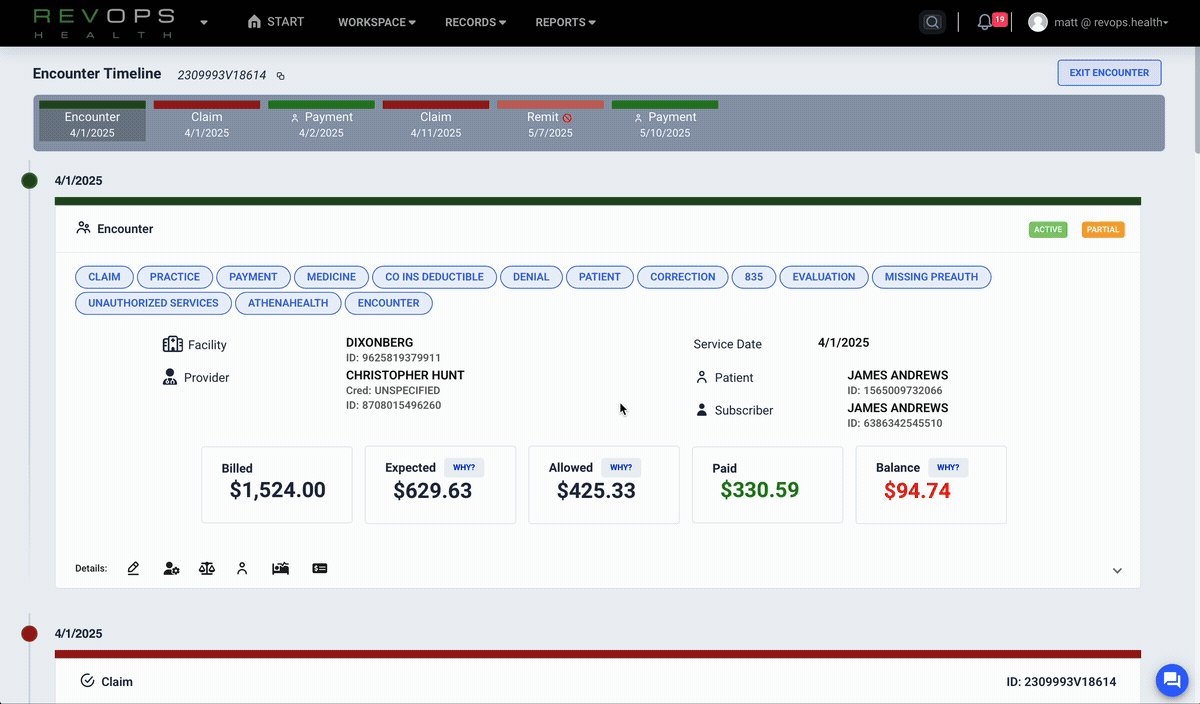
YOUR COMMAND CENTER FOR REVENUE OPERATIONS
Built to give executives, managers, and analysts a shared source of truth.
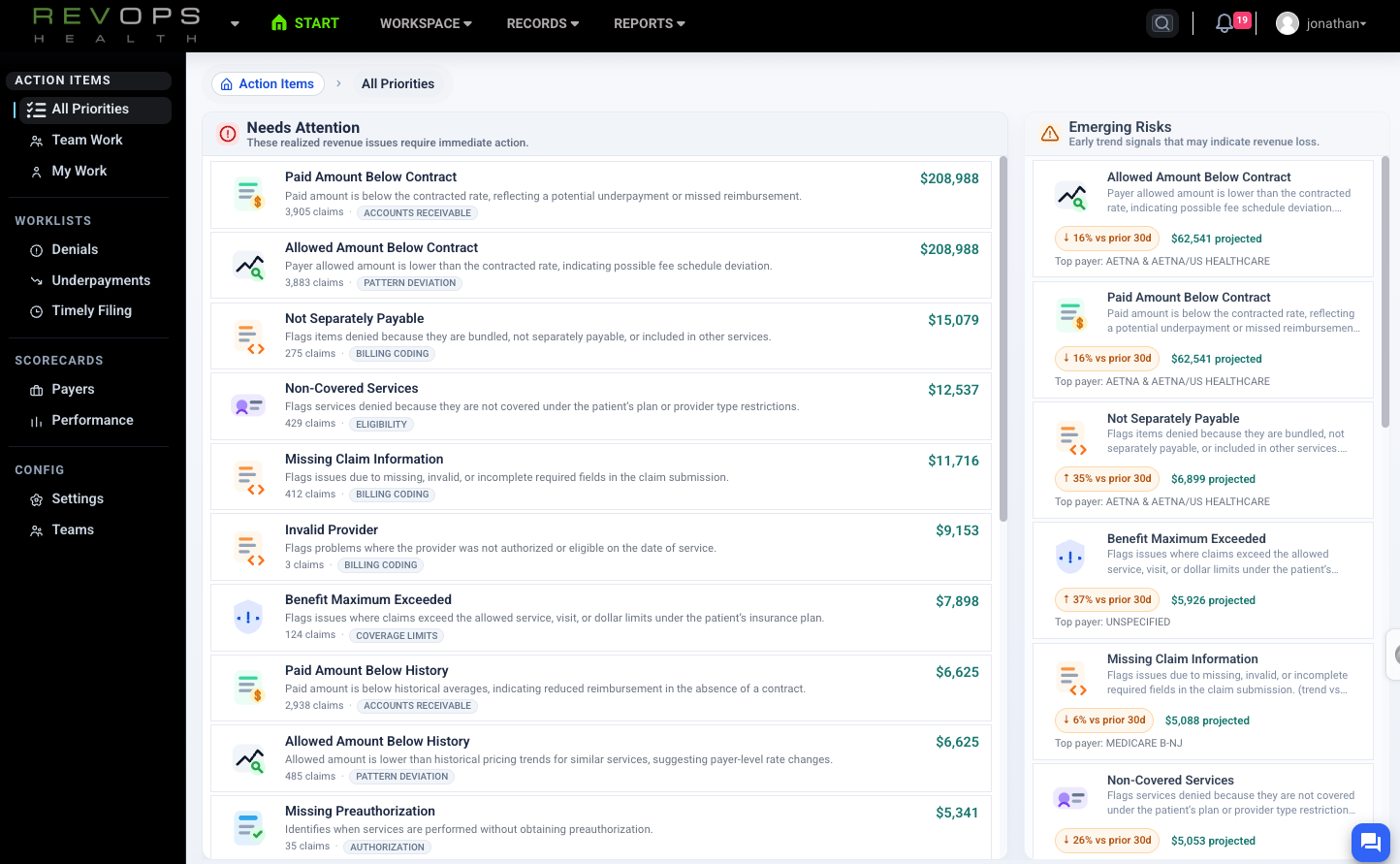
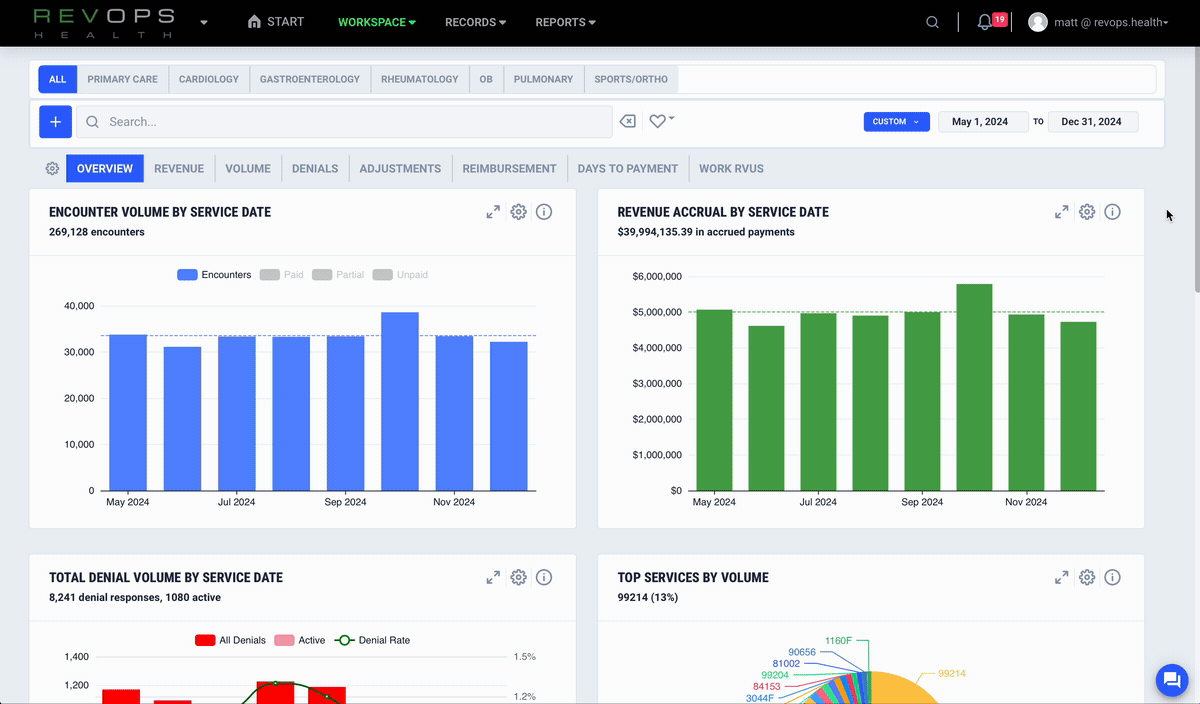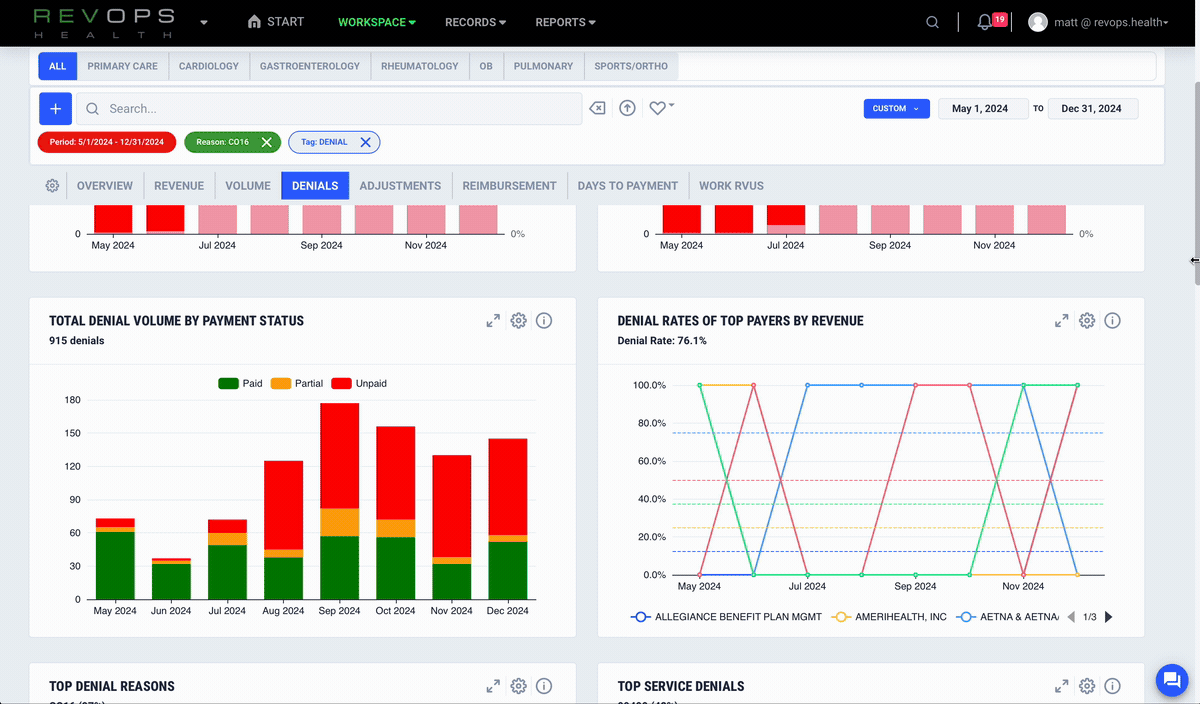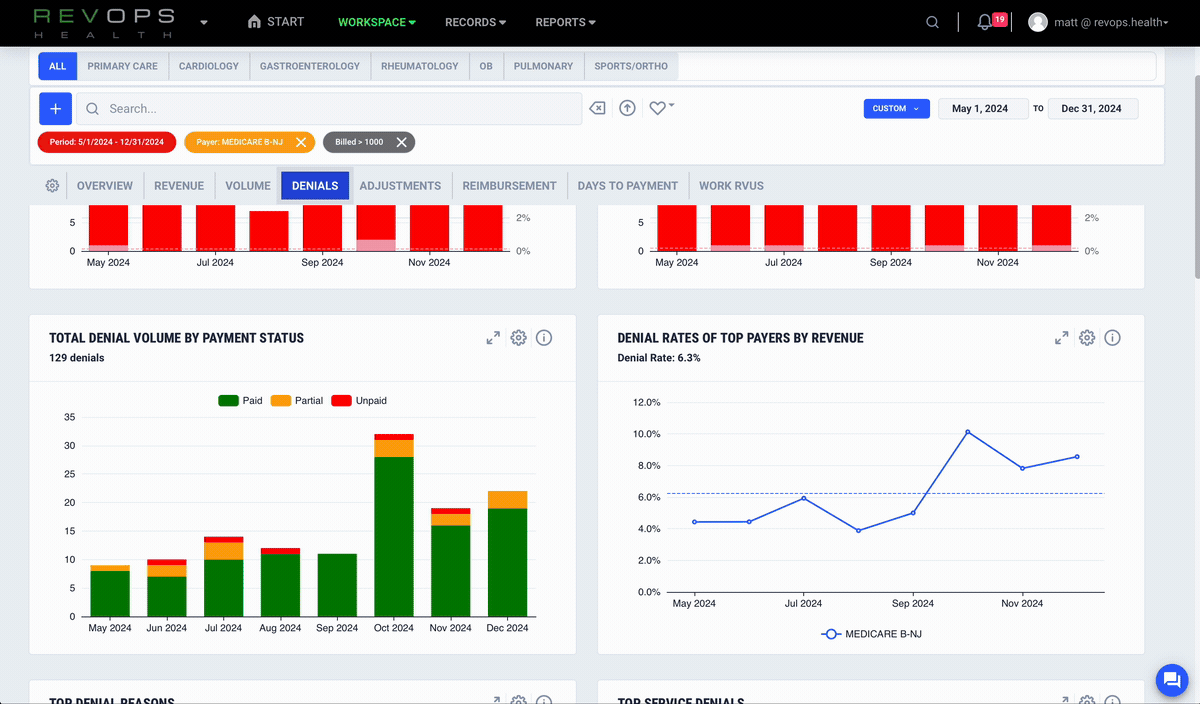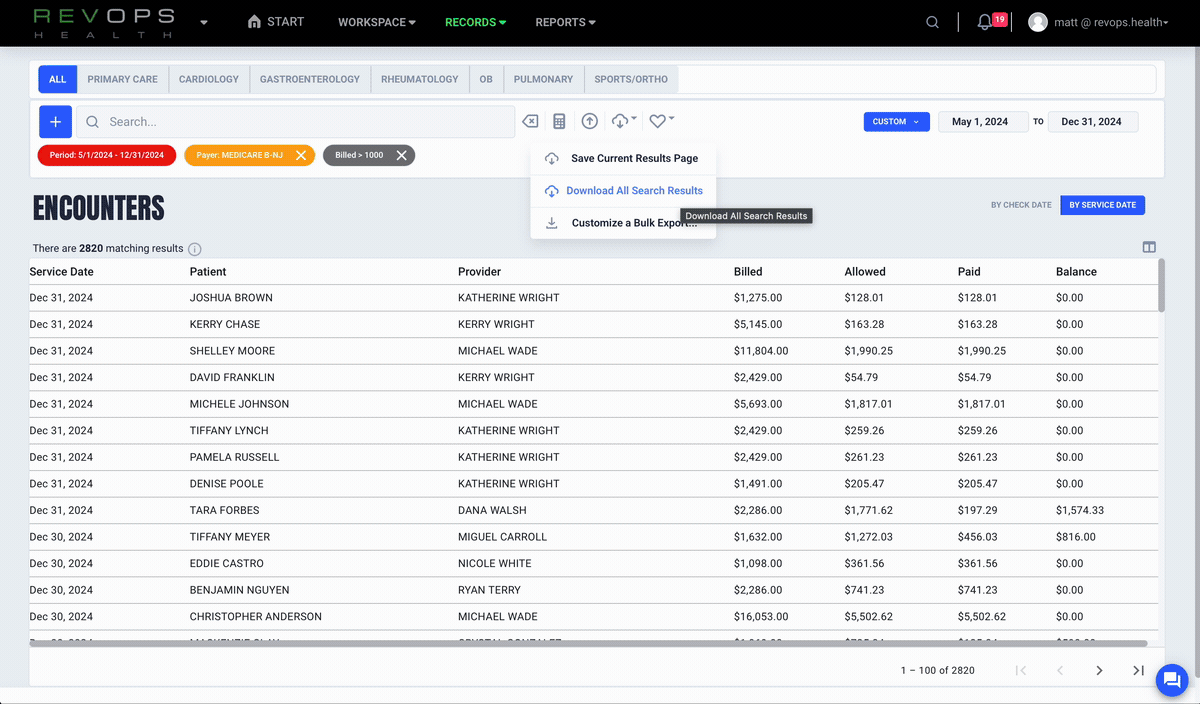
See lost revenue in real time
Enabling customers to identify missing, underpaid, and preventable denied claims as they happen. You see quantified financial impact and get evidence for recovery.
Spot preventable denials instantly
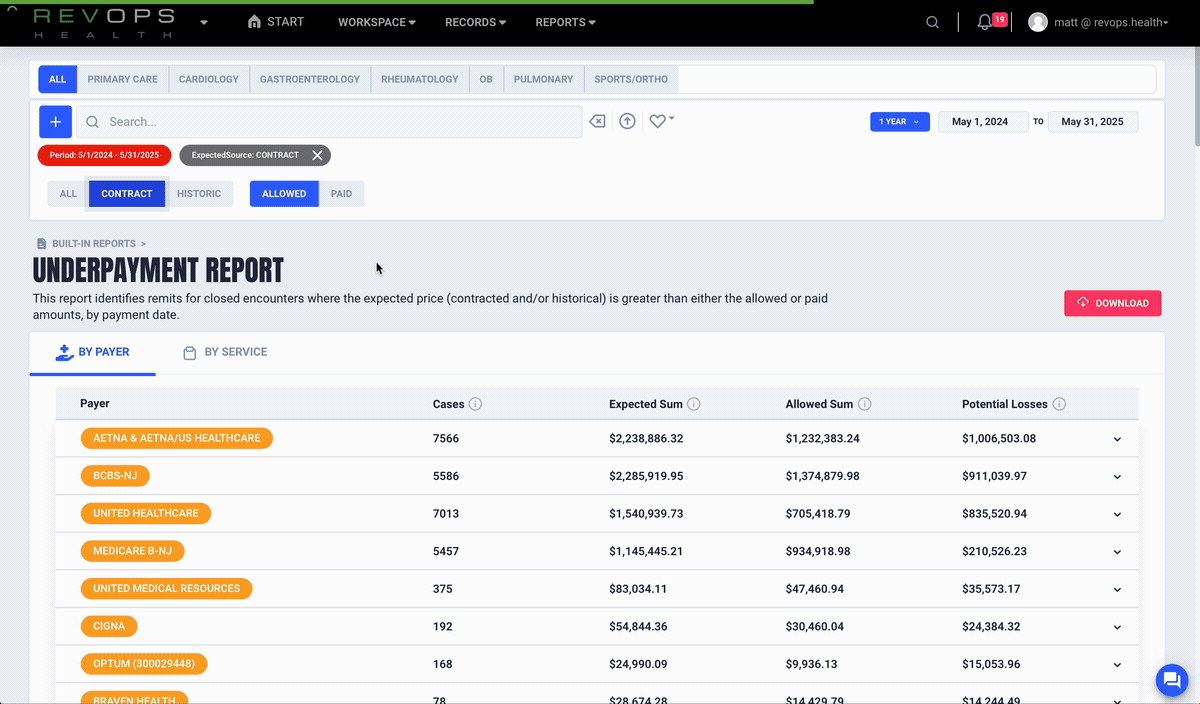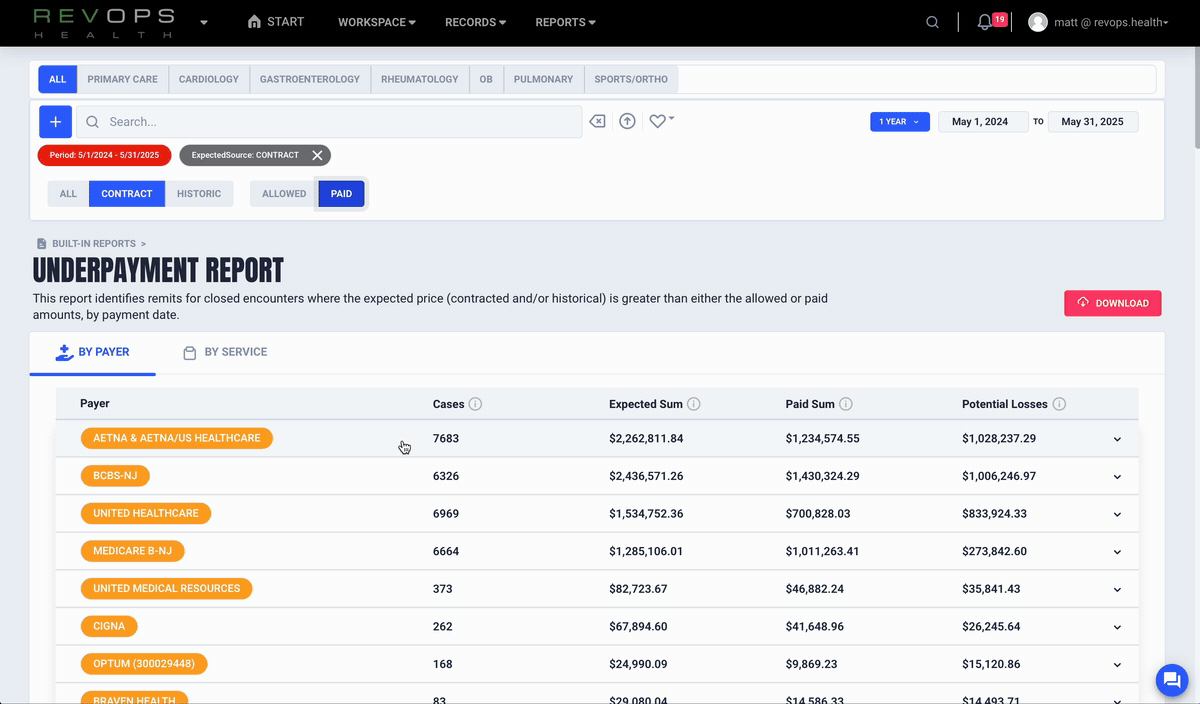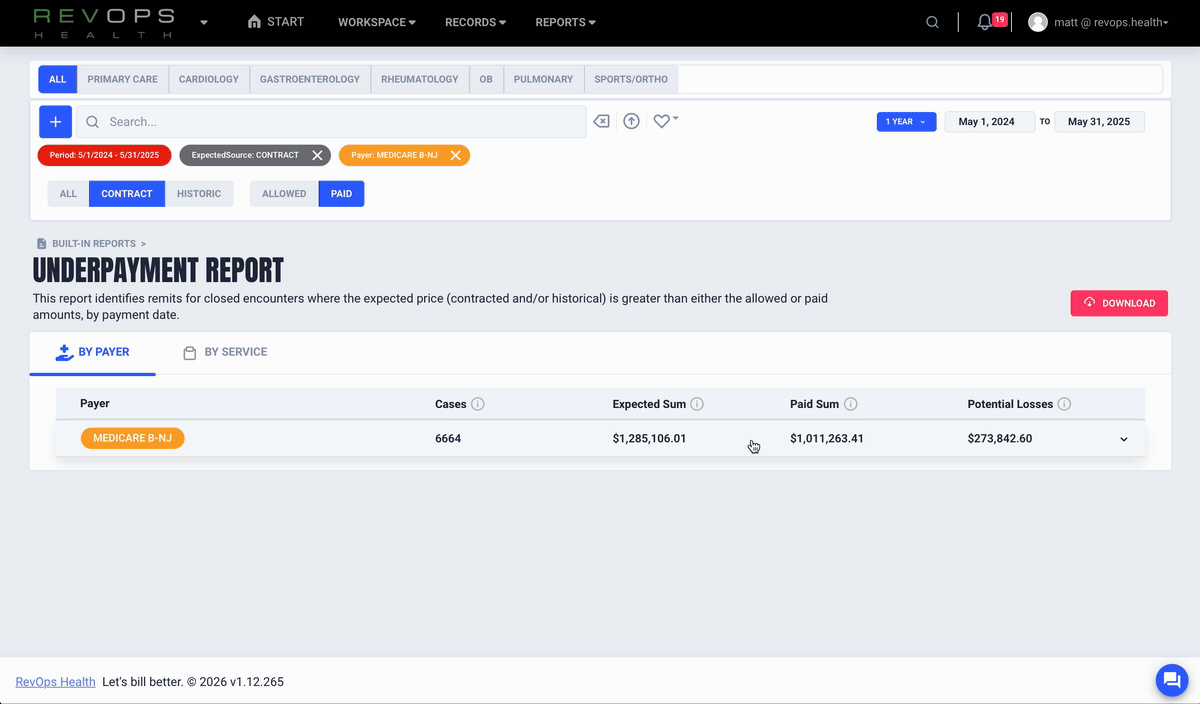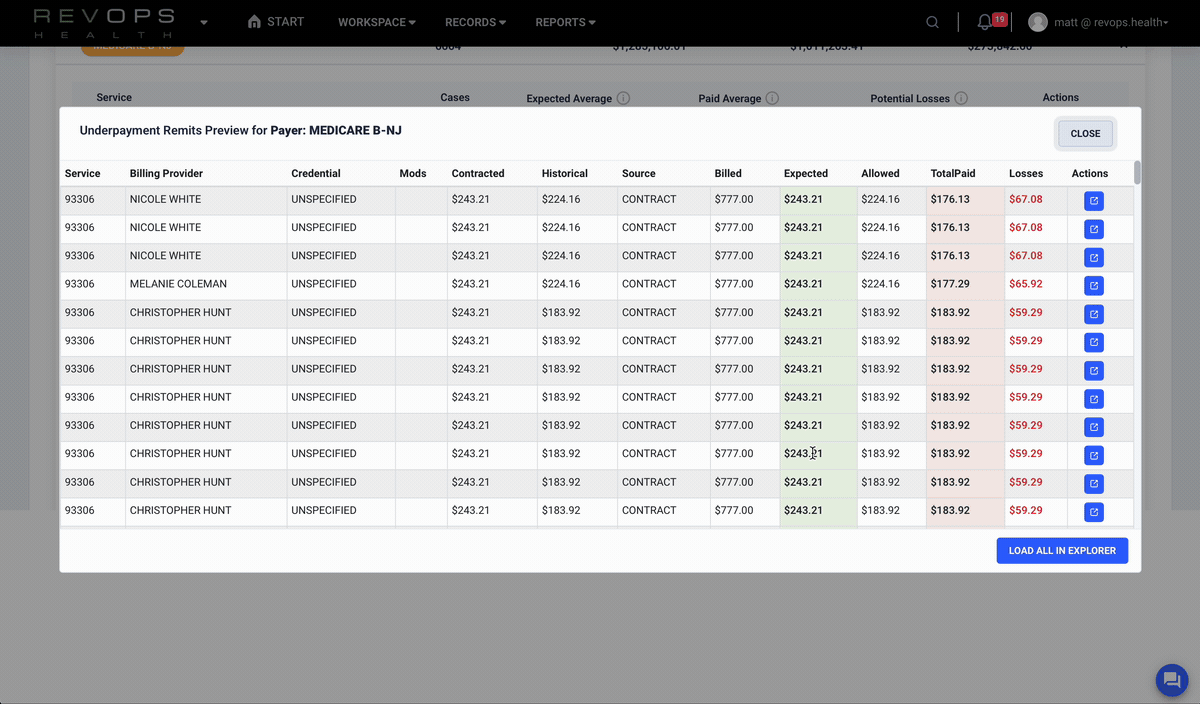
Compare allowed amounts and contracted rates
Identify underpayments
Prioritize high impact issues with real numbers
Detect payer behavior shifts early
The RevOps platform builds a digital fingerprint for each payer and alerts you when reimbursement patterns change so you can respond before cash flow is affected.
Monitor every payer at a service line level
Catch pattern shifts early
Generate evidence packets
Strengthen payer accountability
Understand what drives your KPIs
RevOps connects claims, remittances, and practice data to reveal the drivers behind KPI changes. This makes root cause analysis simple, reliable, and fast.
Reveal operational inefficiencies
Trace problems to their source
Track denial patterns
Improve team performance
Financial clarity
See where revenue is lost and how much can be recovered.
Operational confidence
Understand the real drivers behind performance changes.
Faster decisions
Move from slow reporting to real time insight.
Payer accountability
Catch anomalies early and support every claim with data.
BUILT FOR ANY SPECIALTY, PRACTICE SIZE, OR BILLING MODEL
Independent clinics, provider groups, multi site practices, MSOs, networks, and organizations with limited analytics capacity.